What is an Abdominal Aortic Aneurysm (AAA)?
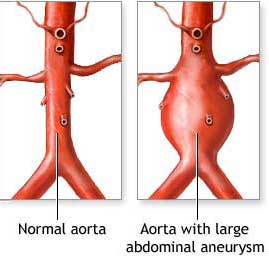
If an artery weakens it will sometimes bulge out and expand. This enlarged area is called an aneurysm. In most cases this is associated with atherosclerosis, but the exact cause is not fully explained. In rare instances aneurysms can occur following trauma to the artery or infections of the blood stream. Aneurysms can affect any artery in the body, but usually occur in specific sites.
The most common site is in the abdominal aorta, the large artery that carries blood from the heart through the abdomen to the legs. Such an aneurysm is called an abdominal aortic aneurysm, more commonly referred to as an AAA or “Triple A”. Aneurysms less commonly occur in the branches of the aorta that go to the legs (the iliac arteries) and in the legs themselves where they enlarge the popliteal artery behind the knee.
At What Age is Someone at Risk?
After the age of 65 a man has a risk of approximately 7%, whereas it less than 1% for a woman. By the age of 80 the risk is up to 10% for a man vs. 2% for a woman. A person’s risk is also increased if a brother or sister has or had an AAA.
How Are AAA Diagnosed?
Aneurysms in the abdominal area enlarge slowly over a period of years. In theory, this means they can be discovered before they cause problems. Unfortunately, aneurysms frequently produce no symptoms before they leak or rupture that would prompt a person to seek medical attention. But they can be picked up at a regular physical examination. For example, an abdominal aneurysm often feels like a throbbing lump under the skin and the patient or an examining doctor may discover the pulsating mass. Even if the lump cannot be felt, the doctor can often hear suspicious sounds of turbulent blood flow through a stethoscope on the abdomen.
When an examining doctor discovers signs suspicious of an abdominal aneurysm, an abdominal X-ray or ultrasound examination may reveal its size and location. More advanced tests, like a CT scan and M.R.I., are usually included in the diagnostic workup. Some vascular specialists, ourselves included, recommend that ultrasound, a simple, quick, non-invasive test, be used to screen people at high risk of abdominal aneurysm. Once an aneurysm has been diagnosed an arteriogram (angiogram) may be required to plan treatment.

What is the Significance of AAA?
The main risk of an aneurysm is that it can rupture resulting in profuse bleeding and often death. Sometimes an aneurysm will fill with blood clot that can break loose causing a blockage in the arterial circulation “downstream”. Accordingly AAA has sometimes been referred to as a “TIMEBOMB IN THE ABDOMEN”.
AAA causes more than 10,000 deaths in the USA and many of these are preventable through early diagnosis and treatment. Approximately 50,000 patients undergo surgery for AAA in the USA alone every year. Once the AAA has ruptured, the chance of dying is 80-90% therefore there are clear-cut reasons for screening for this problem.
Is Screening Justified?
Yes! In the United Kingdom, more than 15000 patients were screened for AAA and there was a subsequent 55% reduction in the incidence of ruptured AAA. In the United States, Medicare will pay for screening in any male who is 65 or older and smoked 100 or more cigarettes in their lifetime. In addition, if the treating physician is suspicious that a patient may have an aneurysm, Medicare/Insurance will insure the test that is ordered to confirm or rule out the diagnosis. For patients who want screening without talking to a physician, we offer a $99 vascular screening exam that evaluates not only for AAA, but also for carotid artery disease and peripheral vascular disease.
How is an Abdominal Aortic Aneurysm Treated?

There is no medical treatment for aneurysms. In general, people with small aneurysms are encouraged to control blood pressure and treat conditions that may accelerate atherosclerosis. Smoking must be curtailed. Exercise is not restricted. There is some experimental work being performed to see whether drugs such as beta-blockers or some antibiotics may slow AAA growth but as yet results have not been encouraging.
There are two methods to repair aneurysms. Both involve surgery.
Open Surgical Repair:
The traditional treatment for AAA is a surgical procedure performed under general anesthetic. An incision is made in the abdomen and the surgeon opens the aneurysm and sews in place a vascular graft to replace the diseased artery. In skilled hands, this procedure can be performed with a mortality of two percent. Patients stay approximately five days in the hospital. They convalesce at home for one week and normally recover fully by six weeks.
Although very rare, complications such as gangrene of the legs, kidney failure, need for a colostomy, pneumonia, and even paralysis can occur. Because this is major surgery, heart attacks may also unusually complicate these operations.
For this reason it is sometimes recommended that patients have a cardiology checkup, which may include a stress test, prior to surgery. In some men sexual dysfunction can occur. Rarely this may be impotence, but in some men a condition known as retrograde ejaculation can result. This implies that vaginal penetration and orgasm still can be achieved, but the semen ejaculates into the bladder rather than externally. This can result in infertility.
It is important to note, however, that once the AAA is repaired by open surgery it is rare that there will be any lasting problems or need for further intervention.
Endovascular Repair:
In this new, less invasive technique, a catheter, or small tube, is inserted into the arteries through a small incision in the groin. Under x-ray guidance, a vascular endograft is delivered through the catheter and placed inside the aneurysm. This endograft fits snugly into the normal artery above and below the aneurysm and so forms a new pathway for the blood to flow thus excluding the aneurysm sac, which then usually goes on to shrink.
Patients go home the next day and frequently are able to resume normal activity by one week. The chance of dying or other complications of AAA repair are lower in endovascular repair compared to open repair. Complications such as gangrene of the leg, claudication, kidney failure, need for colostomy, pneumonia, paralysis and heart attack can also occur with this procedure, however sexual dysfunction should not occur. Unfortunately, not all patients are candidates for this type of procedure.
The vascular surgeon must evaluate each patient on a case-by-case basis. Approximately ten percent of patients may require a further procedure at some stage in the future to fix problems that may develop over time with the graft or the aneurysm sac. Normally, the procedure requires a simple, overnight stay. Long-term surveillance of the patient must be performed usually by means of a CAT scan or ultrasound test. A few patients have ruptured the AAA despite an apparently successful procedure.
Who Should Undergo Treatment?
The risk of aneurysm rupture for aneurysms under five centimeters is quite small. There is not much benefit for surgical intervention for aneurysms of this size. Once the aneurysm reaches five centimeters, the risk of rupture may approximate ten percent per year. Under such circumstances most surgeons would advise repair of the aneurysm unless the patient has prohibitive medical risks against treatment. Although the endovascular treatment is safer than standard surgery most surgeons would still favor withholding this treatment until the aneurysm reaches five centimeters.
Who is at Increased Risk for AAA?
- Male Smokers
- Carotid Disease or Prior Stroke, Ministroke or TIA
- Patients with circulation problems in the legs
- Heart Disease, particularly coronary disease, previous heart attack or heart bypass
- High blood pressure
- Emphysema
For more information please browse the articles below or visit our Articles of Interest.


 Facebook
Facebook
 941-371-6565
941-371-6565  info@veinsandarteries.com
info@veinsandarteries.com