Why dialysis?
The failure of any organ in the body has both physical and emotional consequences. Kidney failure is no exception. However, there are effective ways to cope with the loss of function of your kidneys.
Knowledge concerning the care you receive from your kidney specialist and the dialysis staff can help you to take control of your situation. Controlling your medical condition, however, means that you will have to adopt some new behaviors and lifestyles. Your kidneys did a big job, but now you must consciously make choices to compensate for the role they played in maintaining your health.
The two basic functions of the kidneys are to cleanse the body of waste products and to regulate the amount of water and certain chemicals in the blood. Dialysis helps do both, but watching what you eat and drink and following your doctor’s advice about taking medicines are very important.
What are my treatment options?
Unfortunately, kidney failure is generally irreversible. One option is to have a kidney transplant, but even recipients of a kidney transplant usually must temporarily undergo some form of dialysis. Dialysis is currently practiced in two forms: hemodialysis and peritoneal dialysis.
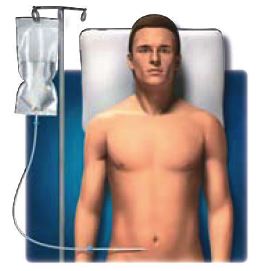
Peritoneal dialysis is conducted through a small tube surgically placed in the lower part of the abdomen. Dialysis fluids are regularly introduced into the abdomen and allowed to remain for several hours. Draining the fluid carries away the body’s chemical waste products.
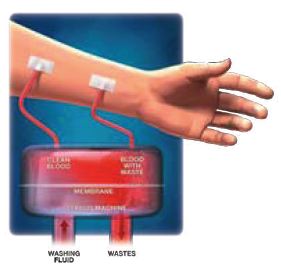
In hemodialysis, blood is removed through a needle and cleansed by running it through a dialysis machine. The blood is returned to the body through a second needle. It can be performed through a catheter or through a dialysis access in the arm or leg.
What are the types of dialysis access surgeries?
Hemodialysis requires access to the blood flowing inside the blood vessels so it can be withdrawn and cleansed. Repeated needle puncture is very hard on veins and arteries, however. Special surgical techniques must be used to create an area that can be used for repeated blood access. Those who are right-handed will often have the left arm chosen for surgery — the right arm for those who are left-handed. If a blood test is ordered before surgery, always ask to have the blood drawn from the arm that will not be operated on. IVs should also be placed in the arm that will not be operated on.
 Catheter:
Catheter:
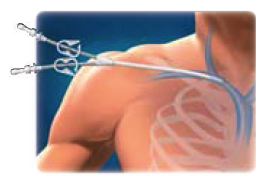
While still in the hospital, most people undergo hemodialysis using a catheter placed into a large vein in the neck region. Since the catheter is placed directly into the circulatory system, it may provide a route for infection and is not a long- term solution. Central Venous Catheters (CVCs) in place longer than two to three months may lead to complications such as vein narrowing or clotting. Long-term hemodialysis patients will need other, longer-lasting solutions. For more information about Living with your Catheter, please click here.
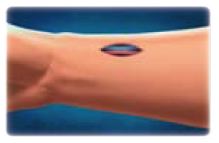
AV Graft:
When the AV graft is implanted, two small incisions are made (AV grafts are commonly placed in the forearm, but they can also be placed in the upper arm or the thigh if necessary). A tunnel is made under the skin to aid in the placement of the graft. One end of the graft is sewn to the artery and the other to the vein. Blood will then flow rapidly from the artery through the graft into the vein.
What is the GORE PROPATEN Vascular Graft?
The GORE PROPATEN Vascular Graft is a special type of vascular graft used to connect the artery with the vein. Similar to other GORE Vascular Grafts, this tube is made from fluoropolymer (expanded polytetrafluoroethylene or ‘ePTFE’). However, the GORE PROPATEN Vascular Graft adds a drug called heparin to the inner surface of the graft. The drug is bonded to the graft surface so that the drug interacts with blood, but does not ‘leak’ into the blood.
Heparin is a drug that prevents blood from clotting and may extend the life of vascular grafts used for dialysis access. Check with your doctor to see if the GORE PROPATEN Vascular Graft is an option for your procedure.
What are the risks of having a fistula or graft placed for dialysis?
There is a risk of infection with any operation. If infection occurs, it can sometimes be treated successfully with antibiotics. However, if the graft gets infected, the graft may have to be removed and another inserted in a different location. If this happens you may also need to have a temporary catheter placed in the area of the neck or groin.
If too much blood flows through the fistula or graft it can steal blood flow to the hand; pain, coldness and numbness may result. This may require reoperation to restrict blood flow through the fistula or graft so that more blood flows to the hand. In some cases, the fistula or graft will have to be divided to prevent it from taking blood flow from the hand. In these situations, a catheter will need to be placed for dialysis.
When can the graft be used?
After the swelling has gone down, you will be able to see the faint outline of the graft in your arm. By placing your fingertips over the graft you will be able to feel a vibration (thrill) that indicates blood is flowing. When you return for your check-up, ask to use your doctor’s stethoscope to listen for the swishing noise (bruit) the blood makes as it flows through the graft. These two signs indicate the AV graft is functioning as intended.
What should I expect during a hemodialysis session?
The first step is to make sure the area where the needle will enter the skin is disinfected. The dialysis technician should wash the site with soap and water, then rub a special antiseptic solution in a circular motion over the area selected. Once this has been done, do not touch the area until after dialysis is complete. Remember that the needle breaks the skin, opening a door for infectious bacteria to enter. Absolute cleanliness is required to reduce your chances of infection.
The technician will then insert the needles through the skin and into the graft or fistula. The needles are taped in place and connected to the lines of the dialysis machine and the dialysis process begins.
When your blood has been sufficiently cleansed of waste products, the technician will remove the needles. To stop the bleeding, the technician may ask you to hold light pressure with a sterile pad. Use just enough pressure to stop the bleeding — too much force may slow the blood flow through the graft or vein and lead to problems.
How long do grafts stay open?
On average, AV grafts stay open about a year. Fistulas tend to stay open for a longer period of time. It is difficult to predict because some grafts become blocked after only a few months while others may stay open for years. You will know when the graft is blocked because the swishing noise and vibration (bruit and thrill) stop. Blockage usually occurs because scar tissue forms where the graft is connected to the vein. This slows the blood flow and produces a clot. When this happens, it is not dangerous, but it does require a procedure to get the clot out. This can generally be performed with catheters and wires.
What will recovery from the surgery be like?
You will experience some bruising, swelling and discomfort in your arm. This is normal and pain medication may be prescribed. Your doctor will give you specific advice, but in general these steps should be followed after you are released from the hospital:
- Keep the arm extended and elevated above the level of the heart; place it on a pillow while lying down and hold it up while sitting.
- Keep the incision area clean and dry; change and replace wet or soiled dressings.
- Avoid putting any pressure on the arm or swinging it around.
- Rest, follow your diet, and take your prescription medicines.
- Your doctor may advise you to perform specific exercises, such as squeezing a ball.
Treatment Tips
To help you get the most out of your treatment, here are some tips on how to spot trouble early and to protect your graft or fistula:
- An infection (figure to right) is a very serious condition. Be sure to keep the area surrounding the graft or fistula clean and always disinfect the puncture site. If a needle puncture site has persistent swelling and redness or any drainage, call your doctor.
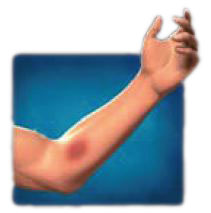
- Do not use a graft or fistula for anything but your dialysis treatments. Your graft or fistula should not be used for blood samples (except during a dialysis session) or intravenous drug treatments.
- Maintain your diet and exercise per your doctor’s instruction. You will feel better and the blood vessels that are your lifelines will be more likely to remain functional.
- A spreading bruise under the skin after the dialysis needle is removed probably means that the bleeding has not stopped. Seek the assistance of your doctor to halt the bleeding.
- A hard knot with black and blue discoloration (figure to right) in any one area of the graft may mean that repeated needle puncture has damaged part of the graft wall. This will need to be repaired. Never allow repeated puncture in the same spot on the graft.
- Do not compress the graft or fistula with tight clothing, bracelets or watches because blood flow might be stopped. Similarly, do not rest a heavy load against it, like a bag of groceries, or sleep on it. And do not have your blood pressure taken in the arm with the graft or fistula because the pressure cuff may stop blood flow.
Reminders
Never
- Never touch the area where the needle is to enter after skin disinfection or during dialysis.
- Never wear tight sleeves, watches, or bracelets over your graft or fistula.
- Never carry heavy loads against or on the graft or fistula (like purses or shopping bags), sleep on it or have blood pressure taken in the same arm.
- Never use your graft or fistula for routine blood tests (except during a dialysis session) or intravenous drug treatments.
Always
- Always make sure your arm is washed and clean before each dialysis session.
- Always follow your doctor’s recommendations for maintaining your diet, taking your prescription medicines and exercising regularly.
- Always apply light pressure to stop bleeding after the dialysis needles are removed. Have the nurse / technician check to make sure bleeding has stopped before you leave the dialysis center.
- Always vary needle puncture sites. Follow a “puncture plan” for advancing needle punctures along the length of the graft before going back to a previous site.
What are the warning signs that a doctor’s care may be needed?
- Swelling, redness, pus drainage or fever may indicate infection.
- A spreading bruise after completion of a dialysis session may indicate graft bleeding under the skin.
- A pulsating hard knot felt under the skin may indicate graft damage because of repeated needle puncturing in the same place.
- Coldness, numbness, aching or weakness of the hand may indicate that not enough blood is getting to the hand (this is not a common problem).
- No vibration (bruit or thrill) from the graft or fistula may mean blood has stopped flowing through it.
Glossary of Terms
Arteriovenous (AV) Fistula
Direct connection between an artery and a vein. The dilated vein is punctured during hemodialysis.
Arteriovenous (AV) Graft
Synthetic material connecting an artery and a vein. The graft is punctured during hemodialysis.
Artery
Vessel carrying blood from the heart to the rest of the body. Bruit ‘Swishing’ sound of blood flowing through an arteriovenous fistula or graft.
Catheter
A tube inserted into a vein to remove blood from the body.
Clot
Blood that thickens and blocks blood flow.
Dialysis
Process of filtering blood to remove toxic materials and to maintain balance of important blood components in the case of impaired kidney function.
Hemodialysis
Removal of toxic substances from the body (dialysis) by removing the blood from the body via tubes directly from an Arteriovenous Fistula or Arteriovenous Graft.
Peritoneal Dialysis
Removal of toxic substances from the body (dialysis) via a catheter placed in the peritoneal cavity.
Thrill
Vibration caused by the flowing of blood through an arteriovenous fistula or graft.
Vein
Vessel carrying blood from the body back to the heart.


 Facebook
Facebook
 941-371-6565
941-371-6565  info@veinsandarteries.com
info@veinsandarteries.com